Boost glp 1 protein: Your Guide to Appetite Control

Some days, hunger makes no sense.
You eat a quick breakfast, then feel distracted by cravings an hour later. Another day, you have eggs, yogurt, or leftovers with more substance, and suddenly the afternoon feels steadier. You're not obsessing over food. You're not white-knuckling your way through meetings. You're just... less hungry.
That difference often gets blamed on willpower, discipline, or “being good.” But your body is running chemistry in the background, and one of the most important signals involved is GLP-1.
If you've heard about GLP-1 because of medications like Ozempic or Wegovy, you're not alone. The topic is everywhere. But the part many people miss is this: GLP-1 is also a natural hormone your body already makes after you eat. And one of the most practical ways to support that natural system is with protein.
That’s where the idea of glp 1 protein becomes useful. Not as a trend phrase, but as a real nutrition tool. When you understand how protein influences fullness, blood sugar, and appetite signals, food choices start to feel less random and more workable.
The Mysterious Feeling of Fullness
A lot of people know this feeling well. Breakfast is toast or a pastry and coffee. It tastes good, goes down fast, and seems like enough in the moment. Then midmorning hits, and suddenly you're looking for something sweet, salty, or crunchy.
On another day, breakfast is Greek yogurt with seeds, or eggs with toast, or tofu with veggies. The meal may not even look much bigger, but your body responds differently. Hunger arrives later. Cravings feel quieter. You can think clearly instead of negotiating with the snack drawer.
That gap matters.
Why two similar meals can feel so different
Your stomach doesn't only care about volume. Your brain doesn't only care about calories. Your gut and pancreas are constantly sending messages about what you ate and what your body should do next.
Some foods trigger a stronger “we’re fed” response than others. Protein is one of the strongest signals in that conversation. It helps activate hormones involved in satiety, including GLP-1, which can help you feel satisfied instead of stuck in a loop of spikes, dips, and cravings.
Practical rule: If a meal leaves you hungry again too soon, that doesn't automatically mean you ate “too much” or “too little.” It may mean the meal didn't send a strong enough satiety signal.
This is why appetite can feel confusing. You can eat enough food and still feel unsatisfied if the meal doesn't match how your body regulates fullness.
A more useful goal than eating less
Many people approach hunger with restriction first. Eat smaller portions. Delay snacks. Ignore cravings. Push through. That approach can work briefly, but it often backfires because it fights symptoms instead of understanding them.
A better question is, “What helps my body register that I’ve eaten?”
That’s where GLP-1 becomes helpful to understand. It helps explain why some meals feel grounding and others leave you chasing more food. And it shows why glp 1 protein isn't about a rigid plan. It's about learning how to work with your biology instead of against it.
Meet GLP-1 Your Body's Smart Messenger
You finish lunch and, on some days, your body seems to get the message. Hunger settles. Food stops taking up so much mental space. On other days, you can eat a similar amount and still feel like something never clicked.
Part of that difference comes from GLP-1.
GLP-1 stands for glucagon-like peptide-1. It is a hormone your intestines release after you eat. Researchers describe it as part of the body’s meal-response system because it helps with insulin release, slows how quickly food leaves the stomach, lowers glucagon, and sends fullness signals that affect appetite in the brain, according to this PubMed overview of GLP-1 physiology.
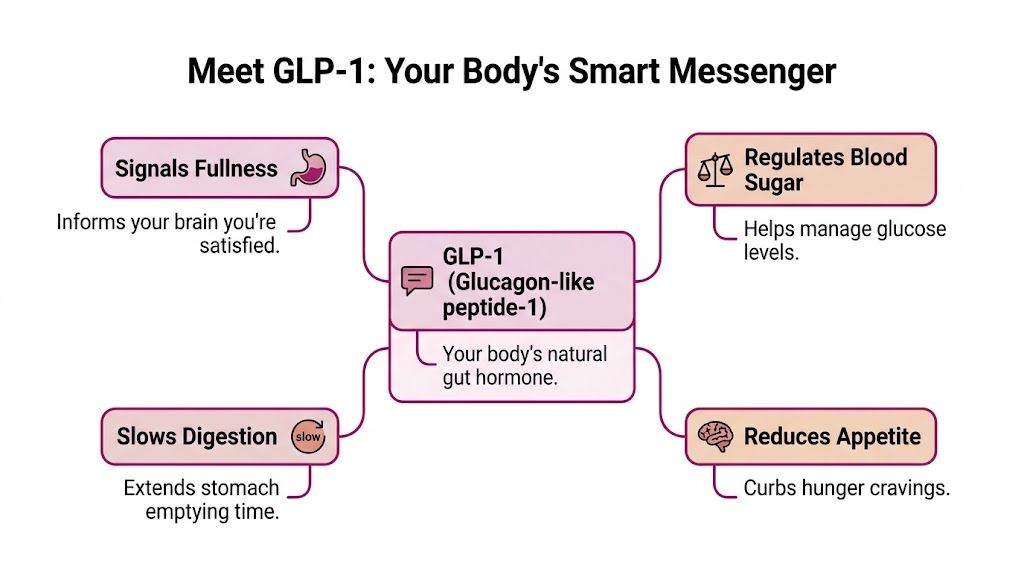
GLP-1 works like a coordinated meal alert
Your body handles a meal the way a good group text works. One message goes out, and several people know what to do next.
After food reaches the gut, GLP-1 helps coordinate the response:
- It signals the pancreas to release insulin when blood sugar rises after a meal.
- It reduces glucagon signaling, which helps keep blood sugar from being pushed upward at the wrong time.
- It slows stomach emptying, so digestion happens at a steadier pace.
- It communicates with the brain, which can increase fullness and lower the drive to keep eating.
That combination helps explain why GLP-1 gets so much attention in both nutrition and medicine. It sits at the intersection of appetite, digestion, and blood sugar control.
Why that matters outside a lab
Hunger is not only about willpower. It is also about signaling.
When this system is working well, eating can feel calmer and more predictable. A meal may stay with you longer. Stopping at comfortable fullness may feel easier. Snacking can feel less urgent, not because you are being more "disciplined," but because your body is giving clearer feedback.
That is a big shift in perspective. It helps explain why the natural GLP-1 hormone and GLP-1 medications are linked in public conversation. The drugs are designed to mimic or extend effects from a hormone your body already uses. The popularity of those medications did not create the biology. It made more people curious about it.
Natural GLP-1 is powerful, even though it is brief
One detail surprises many people. Your own GLP-1 does not stay active for long. Its active form is broken down quickly after release.
That can sound disappointing at first. It is not.
Hormones often act more like text alerts than long meetings. They do not need to stay around all day to matter. They need to show up at the right time, send a clear signal, and start the right response. GLP-1 does that after eating.
Food is part of the signal
GLP-1 responds to nutrients that enter the gut. Carbohydrates, fats, and proteins can all play a role, but protein deserves extra attention because it often creates a stronger satiety response for many people.
That does not mean every meal needs to become high-protein or heavily controlled. It means the makeup of a meal can shape how clearly your body registers, “We have eaten.” For people trying to understand the impact of protein shakes on weight loss, this is part of the reason protein gets so much discussion. It is not only about calories. It is also about signaling.
GLP-1 is one messenger in a larger system. Still, it gives you a useful starting point. If fullness has felt unpredictable, your body is not broken. It may just need meals that send a clearer message.
How Protein Unlocks Your Natural GLP-1
You eat breakfast, feel fine for an hour, then find yourself rummaging through the kitchen before lunch. On another day, a meal with eggs, yogurt, or beans seems to stay with you much longer. That difference is not just about willpower. It is about how clearly your meal tells your gut and brain, “We are fed.”
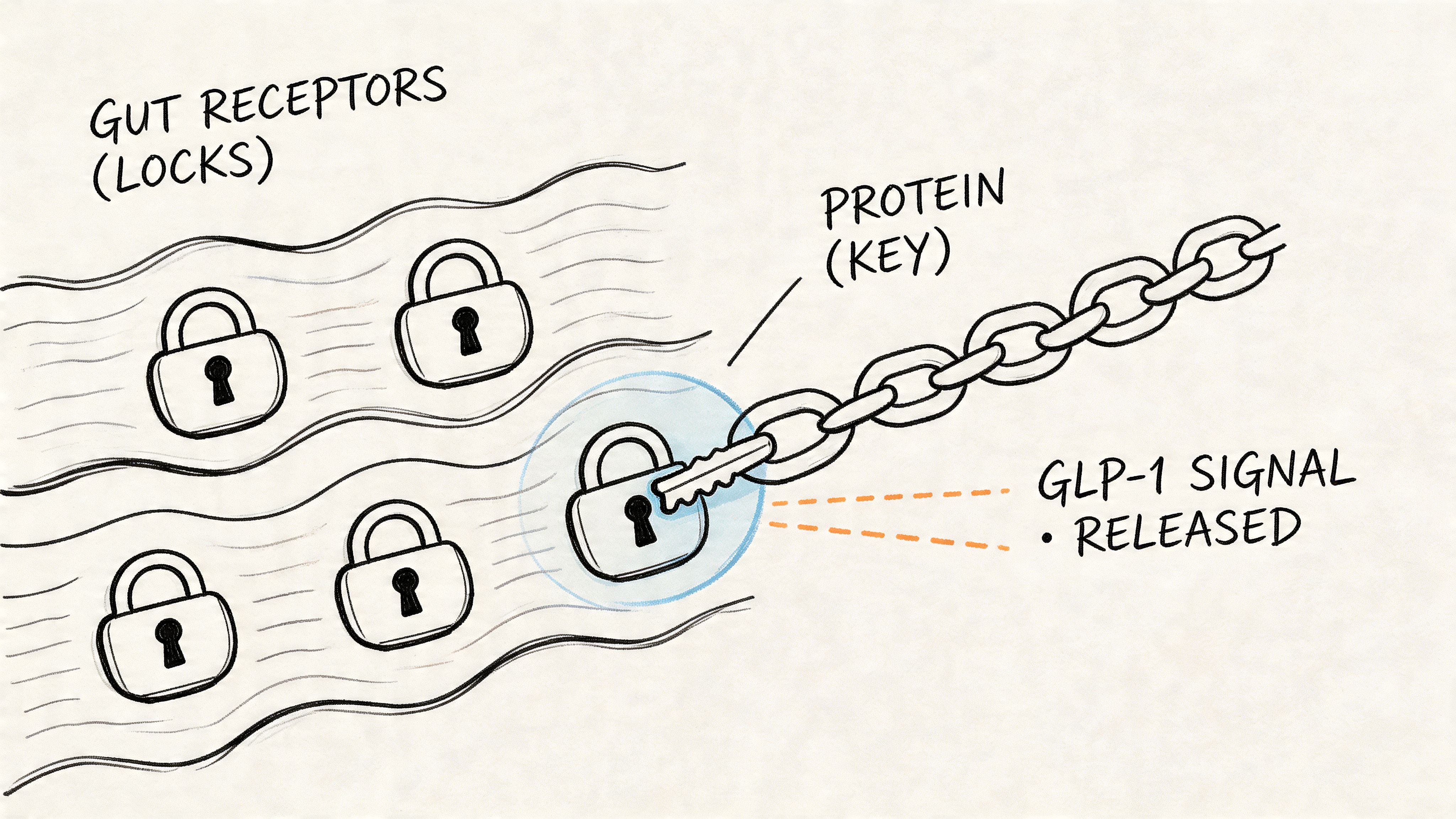
Protein gives the gut a clearer signal
Protein often gets reduced to muscle talk, but it also matters for appetite. As protein is digested, it breaks down into amino acids and small peptides. Cells in the gut respond to those nutrients by releasing hormones involved in fullness, including GLP-1.
A helpful way to picture it is a doorbell, not a switch. Protein does not force fullness all by itself. It presses several signals that help your body register a meal more clearly and slow the rush toward hunger.
That helps explain why protein-rich meals often feel more satisfying than meals built mostly around refined carbohydrates alone. The point is not that carbs are bad. The point is that a meal with some protein usually gives your body more staying power.
You can see that pattern in ordinary meals:
- Eggs and toast often satisfy longer than toast alone.
- Greek yogurt with fruit and nuts usually lasts longer than fruit by itself.
- Lentils, tofu, fish, chicken, cottage cheese, edamame, and beans can all make a meal feel more complete.
Why this matters in the age of GLP-1 drugs
An intriguing aspect emerges. The same GLP-1 pathway that people hear about in medication ads also responds to food. Drugs act on that system in a stronger and longer-lasting way. Meals influence it in a shorter, more natural rhythm.
That does not make food and medication interchangeable. It does help explain why protein keeps showing up in both conversations.
For someone taking a GLP-1 medication, appetite may drop enough that eating becomes easy to postpone. For someone who is not taking one, stress, busy schedules, or erratic meals can create a similar problem. In both cases, each meal has to do more work. It needs to provide nourishment, support fullness, and help protect muscle if total intake is lower.
A meal that blunts hunger but skimps on protein can leave a person underfed in a quieter way, especially over time.
Food first, then convenience if needed
Whole foods are often the easiest foundation because they bring protein along with texture, routine, and other nutrients. But real life counts too. A packed day, low appetite, or limited cooking time can make convenience foods useful.
That is why protein shakes can help some people. They are not magic, and they are not automatically a problem. They are one tool. This guide on the impact of protein shakes on weight loss gives a balanced look at when they help and when they can add extra calories without much satisfaction.
A short visual can help make the connection clearer:
What to focus on in real life
You do not need perfect macros or a high-protein personality. You need meals that include a clear protein source often enough that fullness feels more predictable.
Try using one simple question when building a meal: Where is the protein?
- Animal-based options like eggs, yogurt, fish, chicken, turkey, or cottage cheese
- Plant-based options like tofu, tempeh, edamame, lentils, beans, or higher-protein soy yogurt
- Mixed meals like grain bowls, soups, stir-fries, or wraps where protein is part of the center of the meal
That shift can change the whole tone of eating. Instead of asking, “How little can I get away with?” ask, “What will help this meal satisfy me and support my body?”
The Rise of GLP-1 Drugs and What They Mean
A lot of people first notice GLP-1 through a prescription, not a biology class. They hear a friend say, "I just don't think about food the same way anymore," and wonder whether that means the medication is doing something their body could never do on its own.
The answer is more nuanced. GLP-1 drugs use the same receptor pathway as the natural hormone your body releases after eating, but they do not copy the everyday food response one-to-one. They create a stronger, longer-lasting signal, which is why the effects can feel so different in daily life.
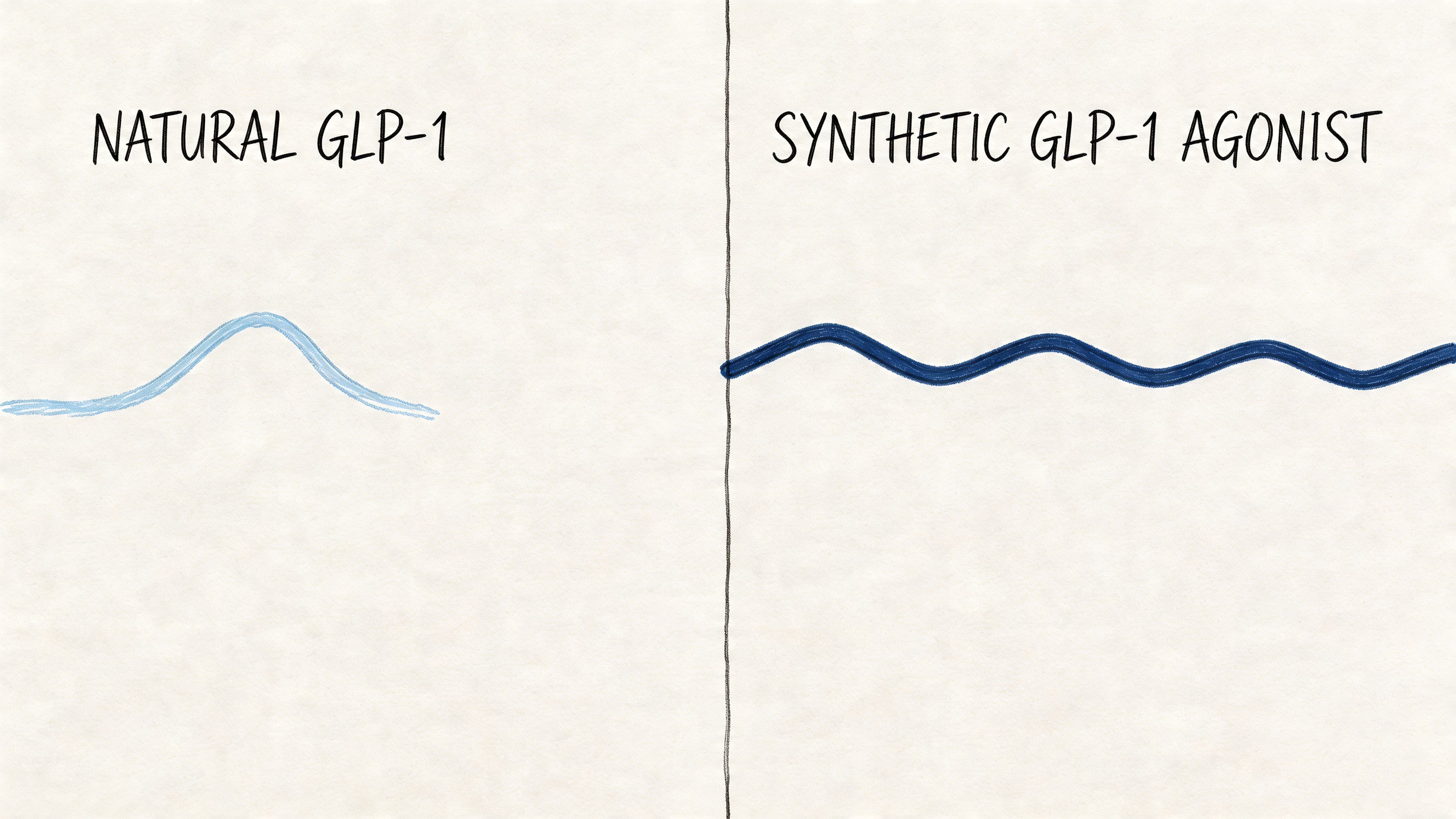
Natural GLP-1 versus medication
Your own GLP-1 works like a short text message after a meal. It helps signal fullness, supports insulin release, and then fades quickly. Medications such as semaglutide are built to stay active much longer, so the appetite signal lasts beyond a single meal.
That longer action helps explain why these drugs have become such a major part of the weight loss conversation. If you're comparing treatment options, this overview of FDA approved weight loss drugs can help you understand the broader medication categories and how they differ.
For some people, that longer signal is life changing. Appetite becomes quieter. Blood sugar feels steadier. The mental noise around food may ease.
For other people, the experience is less dramatic, or harder to tolerate.
Why they are not the same as food-based support
Food and medication can affect the same pathway while still doing very different jobs.
A protein-rich meal asks your body to send its own fullness message. A GLP-1 drug keeps pressing that signal for much longer. One is a normal meal response. The other is a medical intervention designed to extend and strengthen that response.
That difference matters because expectations matter. Someone who starts eating more protein may notice better meal satisfaction and fewer swings in hunger. Someone taking a GLP-1 medication may feel fuller across much of the day, sometimes to the point that eating enough becomes difficult.
A quick comparison makes that easier to see:
| Approach | How it works | What it can feel like |
|---|---|---|
| Natural meal-driven GLP-1 | Brief hormone release after eating | Fuller after meals, steadier appetite |
| GLP-1 receptor agonist drugs | Longer-acting stimulation of the pathway | Lower appetite across the day, earlier fullness |
The nutrition issue that gets missed
Media coverage often stays focused on pounds lost. From a nutrition perspective, a better question is what kind of tissue is being lost.
When appetite drops sharply, people often eat less protein, less total food, or both. That can make it harder to maintain muscle mass, strength, energy, and physical resilience. This is one reason high-protein meals matter during GLP-1 treatment, especially for older adults and for anyone who wants weight loss to come with better function, not just a lower number on the scale.
If a medication reduces appetite, the quality of what you do eat carries more weight.
Why some people respond differently
Response is not identical from one person to the next. Dose, side effects, eating patterns, sleep, stress, genetics, and underlying health conditions can all shape the outcome.
A Stanford report on GLP-1 resistance and genetic variation suggests that some people may be less responsive to this pathway because of inherited differences in how the signal is processed. That helps explain why one person may feel dramatic appetite relief while another says cravings barely changed.
That is not a personal failure. It is a reminder that biology is individual, and treatment decisions work best when they are guided by a clinician rather than hype.
A balanced way to think about them
GLP-1 drugs can be useful medical tools. They can also create practical nutrition challenges, including nausea, early fullness, digestive discomfort, and protein intake that slips too low.
The most helpful frame is simple:
- Medication can reduce appetite
- It does not automatically create nourishing eating patterns
- Protein still matters
- Muscle still matters
- Long-term habits still matter
That perspective connects the science to real life. The natural hormone and the drugs are related, but they are not interchangeable. Understanding that difference helps you use both ideas wisely: medical treatment when it fits, and food habits that support your body every day.
Your Action Plan to Boost GLP-1 with Food
You eat lunch, get full for an hour, then find yourself rummaging for something sweet by midafternoon. That pattern can feel random, but it often has a simple explanation. Meals that are low in protein, rushed, or built mostly around quick-digesting carbs may not give your gut enough support to send a strong, lasting fullness signal.
The good news is that helping your natural GLP-1 response does not require a rigid food plan. It usually starts with meal structure. Protein is one of the clearest places to begin because it supports fullness and helps protect muscle, which matters whether you are trying to eat more steadily on your own or your appetite is lower on a GLP-1 medication.
A practical target for many adults is to make protein a visible part of each meal instead of saving most of it for dinner. That approach tends to work better than treating protein like an afterthought.
Start with the meal itself
Your gut responds to the whole meal, not just one nutrient in isolation. Protein helps. Fiber adds volume and slows digestion. Fat can make a meal more satisfying. Eating pace matters too, because fullness signals are not instant.
| Strategy | Why It Works for GLP-1 | Try This Today with Superbloom |
|---|---|---|
| Lead with protein | Protein can strengthen the fullness response after eating | Log breakfast and notice whether a protein-forward meal changes midmorning cravings |
| Add fiber and some fat | Mixed meals often feel steadier and more satisfying than carbs alone | Take a photo of lunch and check whether it includes a protein source, produce, and a satisfying fat |
| Slow the eating pace | Fullness signals need a little time to catch up with the meal | After dinner, reflect on whether eating more slowly changed how much food felt satisfying |
| Spread protein across the day | A very high-protein dinner may not fully make up for a low-protein morning and lunch | Compare how you feel on days with protein at breakfast, lunch, and dinner versus days when it shows up late |
Three experiments worth trying
Front-load protein at breakfast
Breakfast often sets the tone for the next several hours. If the meal is mostly coffee and refined carbs, hunger can rebound fast. A breakfast with a clear protein source often creates a steadier runway into lunch.
Examples:
- Eggs with toast and fruit
- Greek yogurt with berries and chia
- Tofu scramble with potatoes
- Cottage cheese with fruit and nuts
A useful goal is “more complete,” not perfect.
Build a protein anchor into convenience meals
Busy days expose weak points in eating routines. That is why a protein anchor helps so much. It gives the meal a center of gravity, even if everything else is simple.
That could look like:
- Soup plus edamame
- A sandwich with extra turkey or tofu
- Pasta with beans, chicken, or lentils
- A snack plate with yogurt, fruit, and nuts
Small, repeatable upgrades usually beat dramatic meal makeovers.
Eat slowly enough to notice satisfaction
GLP-1 is part of a larger conversation between your gut and brain. If you eat very quickly, that conversation can get drowned out. Slowing down does not mean turning every meal into a mindfulness exercise. It means giving your body a fair chance to register what is happening.
Try:
- Putting the fork down once or twice during the meal
- Sitting for the meal when possible
- Pausing halfway through
- Asking, “Am I still hungry, or am I still chewing?”
What to do if you're on a GLP-1 medication
The connection between the hormone and the drug has practical implications. The medication may reduce appetite, but your body still needs nourishment. If hunger feels quiet, relying on appetite alone may make it easy to undereat protein or skip meals for too long.
A steadier approach is to focus on:
- Protein first when you do eat
- Gentle, easy foods if your stomach feels sensitive
- Regular opportunities to eat, even when portions are smaller
- Resistance training, if your clinician says it fits your situation, to support muscle retention
For habit support, Superbloom is one option that lets people log meals, reflect on cravings and stress triggers, and notice patterns like low protein or inconsistent meal structure without calorie counting.
Keep the goal realistic
The goal is not to chase a perfect hormone response. The goal is to build meals that leave you nourished, steady, and less vulnerable to the swing from “I forgot to eat” to “now I want everything.”
If you want to improve glp 1 protein support naturally, start with one honest question: where does protein disappear most often in your day? Breakfast is a common place. Lunch at a desk is another. Once you spot the gap, the next step becomes much easier.
Building Sustainable Habits Beyond a Single Hormone
GLP-1 matters, but it isn't the whole story. Hunger, cravings, fullness, stress, sleep, routine, and food environment all interact. That’s why no single hormone can fully explain eating behavior.
Still, understanding GLP-1 gives many people relief. It helps explain why some meals work better than others, why protein is so helpful, and why appetite isn't just about self-control. That shift alone can reduce a lot of shame.
The most sustainable approach is simple. Use protein strategically. Notice how mixed meals affect your energy and hunger. Protect muscle if you're eating less or using a GLP-1 medication. Repeat what helps.
Food works best when it supports your body’s signals instead of fighting them. That’s the value of the glp 1 protein conversation. It turns appetite from a mystery into something you can understand and work with, one meal at a time.
If you want help noticing how protein, meal structure, stress, and hunger patterns connect in real life, Superbloom offers a simple way to reflect on meals, spot patterns, and build steadier habits without strict dieting or calorie counting.